Whitepaper
5
min read
2026 Trends In Patient Payments: Healthcare Financial Experience Study
Subscribe to our newsletter
Stay in the loop in our resources and insights
Thanks for your message!
We will reach back to you as soon as possible.
Patients are the payer with the greatest financial upside
Commercial and government rates are locked in zero-sum agreements. Denials are rising as payers deploy AI to fight claims. Patients are the one payer class where providers can still influence outcomes — and with ACA and Medicaid changes playing out this year, the stakes have never been higher. This report shows which patients are most at risk, where they're getting stuck, and how leading providers are helping them reach resolution before they fall into bad debt.
What's inside
01 — Patient financial risk is hiding in plain sight
The highest-scored accounts may be your biggest collection risk. Cedar analyzed 10 million bills and found that high external propensity-to-pay scores yielded 51% less than bills with no score at all. The signal isn't just noisy — it's working against providers.
02 — Reminders don’t resolve bills — relevance does
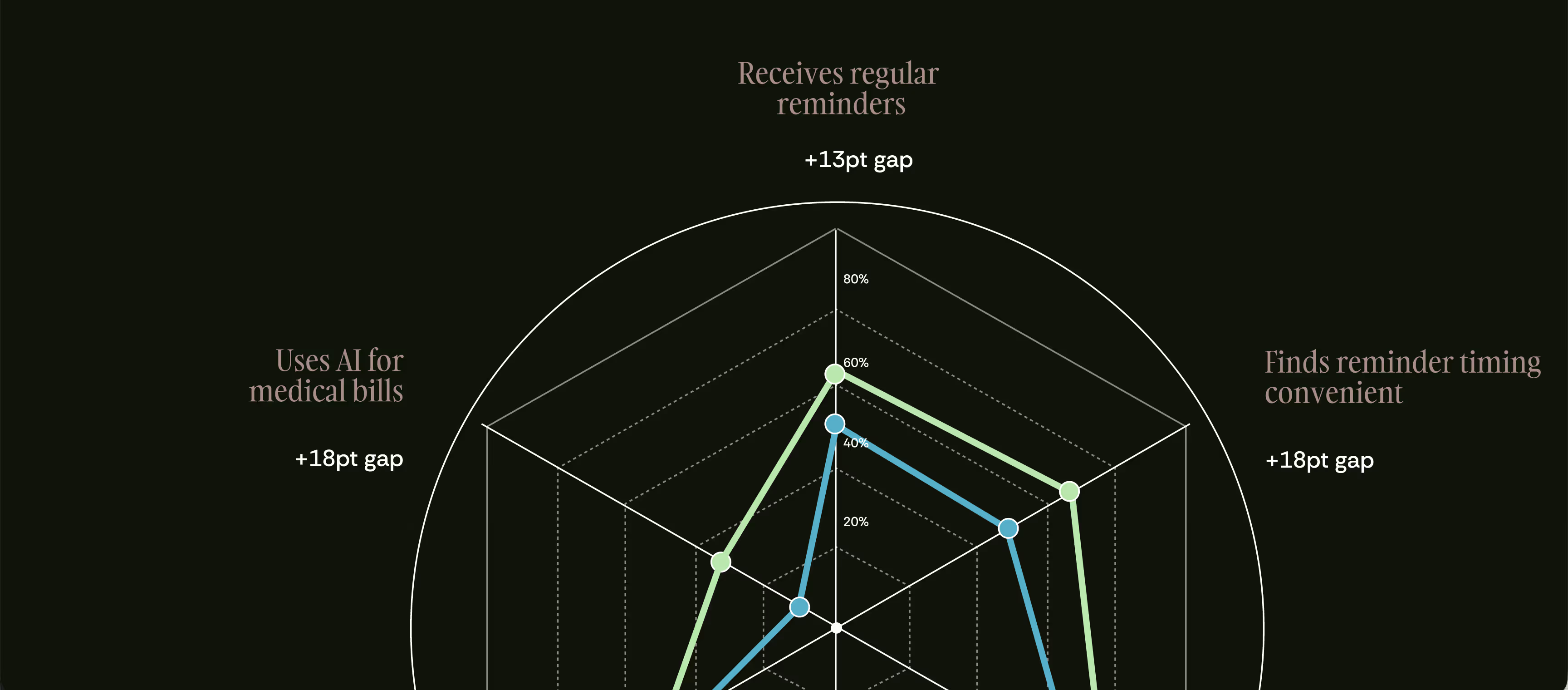
At-risk patients are 3x more likely to report that billing outreach is untimely. But the problem isn't timing — it's what these bills ask at-risk patients to do. When one Cedar partner actually addressed what was blocking payment for a single cohort, collections jumped 17%.
03 — AI is becoming the first stop for billing support
1 in 2 patients have already used AI to interpret their medical bills. They want support on their own terms, after hours, without hold times. The report shows how providers can use their informational advantage to meet that demand and drive resolution.
What the experts say
Get ahead of the coverage shifts hitting your AR in 2026
Providers that see risk clearly, respond precisely, and support patients proactively will outperform those that can't. This report shows what that looks like in practice.









