Some surprises are delightful—your birthday, for instance. Others, however, can result in the worst kind of shock and even prove ruinous.
Surprise billing has been a part of our healthcare system for far too long, with consumers facing unexpected out-of-network costs even when going to in-network facilities for procedures seemingly covered by insurance. A survey by NORC (National Opinion Research Center) at the University of Chicago found that 57% of American adults have been hit with a surprise bill. It’s been far too prevalent, with consumers having no idea how to decipher their insurance benefits, which providers are included in their plan’s network or exactly what is covered. Trying to fight these surprise bills has been even more perplexing and stressful, and often an exercise in futility.
No one should need a doctoral degree to understand what they’re paying for, right?
Enter the No Surprises Act, which went into effect January 2022. While it’s still way too soon to celebrate the end of surprise billing, this legislation is (hopefully) a sign of better days ahead for consumers across the country.
This federal law is designed to shield patients from being blindsided by unexpected medical bills after getting unanticipated out-of-network care in both emergency and non-emergency situations. Now patients are responsible only for cost-sharing amounts they would have been responsible for had the care been in-network.
The change is significant. Healthcare providers face penalties up to $10,000 for each violation of the new regulations. It remains to be seen how compliance will shake out, but one thing is certain: More patients should be relieved of the devastating financial burdens that cause them to forgo care. And that’s a big win for everyone.
Check out our infographic below for more data on surprise billing and the No Surprises Act.
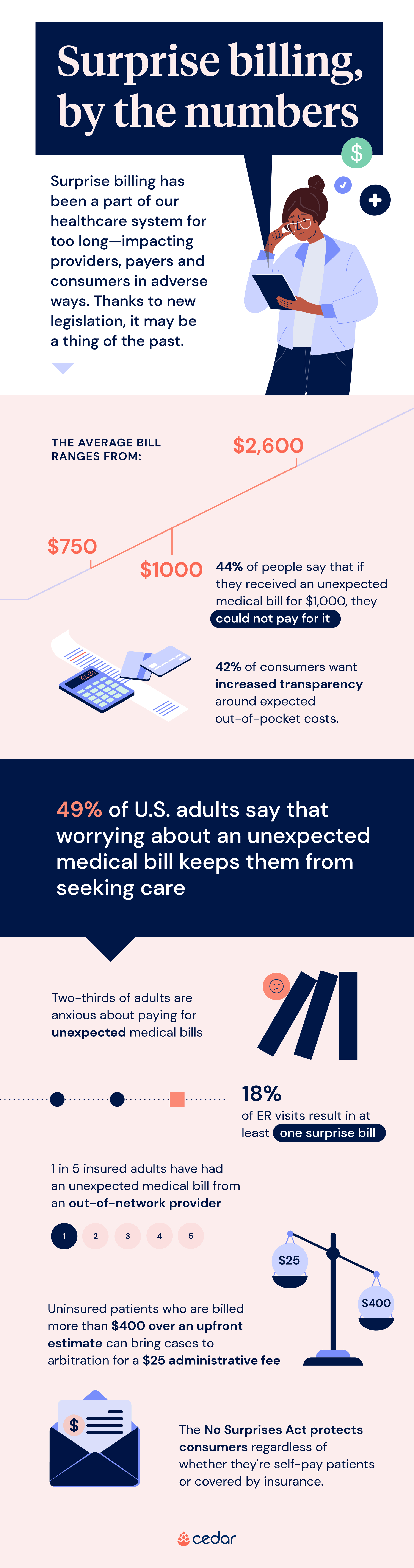
–Journal of the American Medical Association
–Kaiser Family Foundation
–Centers for Medicare & Medicaid Services
–American Heart Association
–Cedar’s 2021 Healthcare Consumer Experience Study



